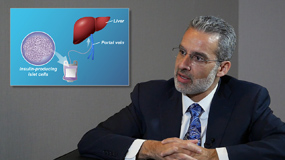
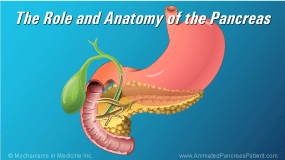
Physicians discuss whether surgery, as well as a number or other types of intervention, can benefit children as treatment options in acute pancreatitis. They explain that in severe cases involving certain types of complications, surgery, interventional radiology, as well as more novel endoscopic approaches can be viable options for consideration. Families may be in contact with a team of specialized care providers ranging from critical care physicians, GI physicians, surgeons, and interventional radiologists, in order to determine the best individualized care for their loved ones.
-
Share with family and friends:
Click here to take our SURVEY
Your feedback is important to us! We will use your feedback to develop future areas of content about pancreatic diseases which will help other patients, caregivers and families.